Many people become physically active to improve their health and to look and feel better. But physical activity may become addictive for a small proportion (3%–5%) of the population. It is important to emphasize that while exercise may represent an addictive behavior for some people who engage in it to an extreme and unhealthy level, habitual exercise itself is not inherently abusive and people should be active to meet guidelines (e.g., 150 minutes of moderate-intensity physical activity per week) to experience its numerous health benefits.
Exercise Dependence Defined
When the desire to exercise becomes an obsession and it negatively impacts a person’s physical and psychological health, it is considered a serious problem known as exercise dependence. Simply stated, exercise dependence is a craving for leisure-time physical activity that results in uncontrollable and excessive exercise behavior that manifests in physiological (e.g., tolerance) or psychological (e.g., withdrawal) symptoms. Other general terms for exercise dependence include exercise addiction, overexercising, obligatory exercise, compulsive exercise, and exercise fanaticism. Common characteristics of exercise dependence are continuing to exercise despite having an injury or illness; giving up social, occupational, and family obligations for exercise; and experiencing withdrawal effects, such as anxiety and tension when not able to exercise.
Academic Writing, Editing, Proofreading, And Problem Solving Services
Get 10% OFF with 24START discount code
The growing consensus in recent years is that exercise dependence is similar to other substance dependence disorders and should be defined within a cluster of cognitive, behavioral, and physiological symptoms. Researchers have thus defined exercise dependence as a maladaptive pattern of exercise, leading to clinically significant impairment or distress, as manifested by three (or more) of the criteria listed in Table 1, occurring at any time in the same 12-month period.
Exercise dependence may also play a pivotal role in explaining the function of exercise behavior in the development and maintenance of eating disorders. To this end, it is necessary to distinguish the etiology of the exercise dependence symptoms. Understanding the psychological antecedents of exercise may help clarify the relationship between eating disorders and excessive exercise by offering insight into the distinction between primary versus secondary exercise dependence. Primary exercise dependence occurs when the individual meets criteria for exercise dependence and continually exercises solely for the psychological gratification resulting from the exercise behavior—for example, a runner who continually increases distance and speed to facilitate the enjoyment that is experienced from the running itself. Secondary exercise dependence occurs when an exercise-dependent individual uses increased amounts of exercise to accomplish some other end, such as weight management or body composition manipulation—for example, a runner who continually increases distance and speed to burn calories and facilitate weight loss. Because exercise can be used as a compensatory behavior to either prevent or reverse weight gain, secondary exercise dependence in the context of eating disorders occurs when an individual meets the criteria for exercise dependence and continually exercises to manipulate and control one’s own body; thus, exercise dependence is secondary to an eating disorder. Recently, researchers have found that exercise dependence symptoms, not exercise behavior, mediate the relationship between exercise and eating pathology. That is, psychological factors, rather than the amount of exercise itself, may better explain why the exercise dependence–eating disorder relationship exists.
Prevalence and Societal Importance of Exercise Dependence
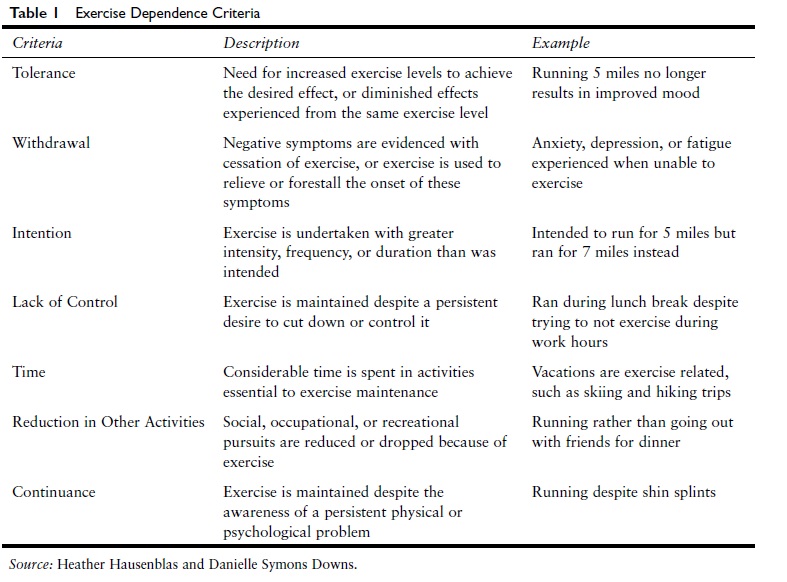
Table 1 Exercise Dependence Criteria
Despite the worldwide increase in obesity over the past several decades, there is nevertheless a growing rate of excessive behavioral addictions, such as gambling; Internet use; and exercise dependence that can result in poor psychological and physiological health outcomes, including increased risk for illness, stress, depression, and injury. Recent evidence suggests the estimated prevalence of exercise dependence in the general adult population is 3% to 5%. Among particular subgroups of adult exercisers, for example marathoners and sport science students, the prevalence of exercise dependence is even higher. In general, men present higher rates of exercise dependence symptoms, which parallels the higher rates of physical activity participation among men than women. The prevalence rate is about 10% for at risk for exercise dependence among regular adult exercisers. Even more concerning is the recent evidence that youth may also be at risk for exercise dependence symptoms. One study found that 6% of youth ages 14 to 16 years were classified as at risk for exercise dependence and an additional 65% were classified as nondependent but with some symptoms. Compared to the girls, the boys reported more overall exercise behavior and exercise dependence symptoms. While it has historically been thought that men develop exercise dependence symptoms in early adulthood as they hit their peak fitness level, this recent evidence suggests that boys may be more at risk for developing exercise dependence symptoms at an earlier age in the developmental timeline—possibly due to their greater involvement in leisure-time play, youth sports, and the types of vigorous activities like running and weight lifting that can perpetuate overexercising. This is problematic because it increases the chances for long-term chronic health problems (injury, illness).
There is also a growing body of research beginning to quantify the exact aspects of health that are affected by exercise dependence. Specifically, compared with nondependent controls, individuals with exercise dependence often experience an increased amount of overuse injuries like tendinitis and muscle injuries, negative affect (particularly during exercise cessation), anxiety about the shape of one’s body, neuroticism, hypochondria, and compulsive shopping or buying. Unfortunately, exercise dependence tends to be overlooked because it represents a socially acceptable (or socially tolerated) addiction that appears to be a reasonable form of dependence.
Measurement of Exercise Dependence
Measurement of exercise dependence relies primarily on self-report assessments due to the manifestation of psychological, behavioral, and cognitive symptoms. Assessing the frequency, duration, and intensity of physical activity alone does not provide an accurate estimate of the underlying psychological factors that drive the symptomatology. Although there are several unidimensional measures of excessive exercise (e.g., Negative Addiction Scale, Commitment to Running Scale, and Obligatory Exercise Questionnaire), these measures have been criticized for not providing a complete assessment of the construct of exercise dependence.
The growing consensus among researchers and practitioners is that exercise dependence is better conceptualized as a multidimensional construct that parallels behavioral addiction, and therefore, is more appropriately measured by multidimensional assessments that take into account the theoretical underpinnings of addiction. Researchers have posited that behavioral addictions manifest when a behavior can provide either pleasure or relief from internal discomfort of anxiety or stress, and the behavior is characterized by feelings of powerlessness or loss of control, and is maintained despite serious physical or psychological consequences. It is now accepted that addictions are a part of a biopsychosocial process that share a set of common symptoms, such as tolerance, withdrawal, mood modification, conflict, and relapse.
One validated self-report measure that falls within this categorization of addiction is the Exercise Addiction Inventory (EAI) developed by Annabel Terry, Attila Szabo, and Mark Griffiths. The EAI assesses six components of exercise addiction: salience, mood modification, tolerance, withdrawal, conflict, and relapse. Another psychometrically validated measure to assess exercise dependence is the Exercise Dependence Scale-Revised (EDS-R) developed by Heather Hausenblas and Danielle Symons Downs and is based on the Diagnostic and Statistical Manual of Mental Disorders, 4th Edition, Text Revision (DSM-IV) criteria for substance dependence. This 21-item measure assesses symptoms across seven criteria (tolerance, withdrawal, intention effects, loss of control, time, reduction in other activities, and continuance). The EAI and EDS-R are easy to administer and offer researchers and practitioners useful tools for assessing exercise dependence symptoms.
Exercise Dependence Diagnosis and Treatment
Currently there are no formal diagnostic criteria for exercise dependence. However, the DSM-IV now includes behavioral addictions (although gambling is the only designated behavioral addiction in this category). A key factor in identifying a person with exercise dependence symptoms is distinguishing between the excessive exercise behavior and eating pathology. As noted above, primary exercise dependence occurs in the absence of an eating disorder, whereas secondary exercise dependence co-occurs with eating pathology. Thus, a diagnostic hierarchy is required whereby a person should be first evaluated for an eating disorder such as anorexia nervosa or bulimia nervosa. If the exercise behavior is secondary to the eating pathology, then referral and treatment for an eating disorder should be the priority. If eating pathology is ruled out, the individual may meet the criteria for primary exercise dependence. However, focusing only on the excessive exercise behavior in terms of frequency and intensity of exercise patterns fails to take into account the criteria that are unique to substance dependence, such as tolerance and withdrawal. Thus, determining if a person meets the aforementioned criteria for exercise dependence may provide insight to the excessive exercise. Both the EAI and EDS-R are reliable and useful tools that may assist clinicians in assessing exercise dependence. Also considering other coexisting addictions, such as alcohol or drugs or behavioral addictions like gambling, spending, or Internet use, can provide additional context to whether the person has an addictive personality disorder. Identifying individuals who are at risk for exercise dependence is a major challenge because exercise is considered a positive health behavior. Thus, excessive exercise often goes unnoticed as a negative health behavior until it has reached an extreme form. A key warning sign to distinguish between healthy and dependent exercise is that healthy exercisers organize their exercise around their lives, whereas dependents organize their lives around their exercise.
References:
- American Psychiatric Association. (2000). Diagnostic and statistical manual of mental disorders (4th ed., text revision). Washington, DC: Author.
- Cook, B. J., & Hausenblas, H. A. (2008). The role of exercise dependence for the relationship between exercise behavior and eating pathology: Mediator or moderator? Journal of Health Psychology, 13, 495–502.
- Griffiths, M. D. (2005). A “components” model of addiction within a biopsychosocial framework. Journal of Substance Use, 10, 191–197.
- Hausenblas, H. A., & Symons Downs, D. (2002). Exercise dependence: A systematic review. Psychology of Sport and Exercise, 3, 89–123.
- Hausenblas, H. A., & Symons Downs, D. (2002). How much is too much? The development and validation of the exercise dependence scale. Psychology & Health, 17, 387–404.
- Monok, K., Berczik, K., Urban, R., Szabo, A., Griffiths, M. D., Farkas, J., et al. (2012). Psychometric properties and concurrent validity of two exercise addiction measures: A population wide study. Psychology of Sport and Exercise. Retrieved from http://dx.doi.org/10.1016/j.psychsport.2012.06.003
- Symons Downs, D., DiNallo, J. M., & Savage, J. S. (2013). Self-determined to exercise: Leisure-time exercise behavior, exercise motivation, and exercise dependence symptoms in youth. Journal of Physical Activity and Health, 10, 176–184.
- Symons Downs, D., Hausenblas, H. A., & Nigg, C. R. (2004). Factorial validity and psychometric examination of the Exercise Dependence ScaleRevised. Measurement in Physical Education and Exercise Science, 8, 183–201.
- Terry, A., Szabo, A., & Griffiths, M. D. (2004). The exercise addiction inventory: A new brief screening tool. Addiction Research and Theory, 12, 489–499.
See also: