Theories of health behavior change are needed to explain, predict, and improve self-regulation of physical activity. Such theories are being divided into continuum models and stage models. In continuum models, people are positioned along a range that reflects the likelihood of action. Influential predictor variables are identified and combined within one prediction equation. The goal of an intervention is to move the person along this route toward action. Health promotion, then, focuses on increasing all model-inherent variables in all persons, without matching treatments to particular audiences. The theory of planned behavior (TPB), developed by Icek Ajzen, is one such continuum model.
In contrast, according to stage models, health behavior change consists of an ordered set of categories (or stages) into which people are classified. These categories reflect cognitive or behavioral characteristics, such as the intention to perform a behavior. The main purpose of applying stage models lies in the identification of relatively homogeneous target groups for interventions and the design of stage-matched treatments. The most popular stage theory of health behavior change is the transtheoretical model (TTM), developed by James Prochaska, that proposes five stages of change.
Both continuum models and stage models have their advantages and disadvantages. Continuum models have been found useful for explanation and prediction, whereas stage models are often preferred to guide interventions. For health promotion, the continuum models are often too general because all variables involved in such a model need to be addressed in interventions, without considering the special needs of particular subgroups of participants. However, it is possible to integrate both approaches when researchers use a continuum model as a theoretical template and, when it comes to interventions, subdivide the audience into stage groups to allow for stage-matched treatments. The health action process approach (HAPA), developed by Ralf Schwarzer, is such a hybrid model with a continuum layer as well as a stage layer.
Mediating Mechanisms
The traditional continuum models have been criticized mainly because of the so-called intention– behavior gap (referring to the frequent failure of intention to predict behavior). HAPA explicitly includes postintentional factors to overcome this gap. It suggests a distinction between (1) preintentional motivation processes that lead to a behavioral intention, and (2) postintentional volition processes that lead to the actual health behavior. Within the two phases, different patterns of social cognitive predictors may emerge (see Figure 1). In the initial motivation phase, a person develops an intention to act. In this phase, risk perception is seen as a distal antecedent (e.g., “I am at risk for cardiovascular disease”). Risk perception in itself is insufficient to enable a person to form an intention. Rather, it may set the stage for a contemplation process and further elaboration of thoughts about consequences and competencies. Similarly, positive outcome expectancies (e.g., “If I exercise five times per week, I will reduce my cardiovascular risk”) are chiefly seen as being important in the motivation phase, when a person balances the pros and cons of certain behavioral outcomes. Further, one needs to believe in one’s capability to perform a desired action, perceived self-efficacy (e.g., “I am capable of adhering to my exercise schedule in spite of the temptation to watch TV”). Perceived self-efficacy operates in concert with positive outcome expectancies, both of which contribute to forming an intention. Both beliefs are needed for forming intentions to adopt difficult behaviors such as regular physical exercise.
After forming an intention, the volitional phase is entered. When a person is inclined to adopt a particular health behavior, the good intention has to be transformed into detailed instructions on how to perform the desired action. Once an action has been initiated, it has to be maintained. This is not achieved through a single act of will but involves self-regulatory skills and strategies. Thus, the postintentional phase is further broken down definition that includes irreversibility and invariance. The terms phase or mindset may be equally suitable for this distinction. The basic idea is that individuals pass through different phases on their way to behavior change. Thus, interventions may be most efficient when tailored to these particular mindsets.
For example, preintenders are supposed to benefit from confrontation with outcome expectancies and some level of risk communication. They need to learn that the new behavior like becoming physically active has positive outcomes, such as well-being, weight loss, and fun, as opposed to into more proximal factors, such as planning, coping self-efficacy, and recovery self-efficacy. Additional volitional constructs that have been included in HAPA research are action control and social support.
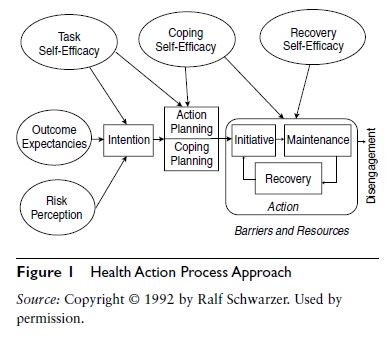
Figure 1 Health Action Process Approach
Including planning and self-efficacy as volitional mediators renders the HAPA into an implicit stage model because it implies the existence of at least a motivational and a volitional phase. The purpose of such a model is twofold: It allows a better prediction of behavior, and it reflects the assumed causal mechanism of behavior change. Research that is based on this continuum layer of the model employs path-analytic methods.
Preintenders, Intenders, Actors
When it comes to the design of interventions, one can consider turning the implicit stage model into an explicit one. This is done by identifying individuals who are located either in the motivational stage or in the volitional stage. Then, each group receives a specific treatment that is tailored to this group. Moreover, it is useful and theoretically meaningful to subdivide the volitional group further into persons who perform and those who only intend to perform. In the postintentional– preactional stage, individuals are labeled intenders, and in the actional stage actors. Thus, a pragmatic subdivision within the health behavior change process yields three groups: preintenders, intenders, and actors.
The term stage in this context was chosen to allude to the stage theories, but not in the strict the negative outcomes that accompany the current (sedentary) behavior, such as developing an illness or being overweight. They also need to develop an optimistic belief that they are capable of performing the critical behavior.
In contrast, intenders should not benefit much from health messages in the form of outcome expectancies because, after setting a goal, they have already moved beyond this mindset. Rather, they should benefit from planning to translate their intentions into action.
Finally, actors should be prepared for particular high-risk situations in which lapses are imminent. Interventions help them if they desire to change their routines by adopting or altering a behavior, for example.
Five Principles
The HAPA is designed as an open architecture that is based on principles rather than on specific testable assumptions. Developed in 1988, it was an attempt to integrate the model of action phases by Heinz Heckhausen and Peter Gollwitzer, with social cognitive theory developed by Albert Bandura, based on five principles.
Principle 1: Motivation and volition. The health behavior change process is divided into two phases. There is a switch of mindsets when people move from deliberation to action. First comes the motivation phase in which people develop their intentions. Afterwards, they enter the volition phase.
Principle 2: Two volitional phases. In the volition phase, there are two groups of people: those who did not yet translate their intentions into action, and those who did. Thus, there are inactive as well as active persons in this phase. In other words, in the volitional phase one finds intenders as well as actors who are characterized by different psychological states. In addition to health behavior change as a continuous process, one can also create three categories of people with different mindsets, depending on their current location within the course of behavior change: preintenders, intenders, and actors.
Principle 3: Postintentional planning. Intenders who are in the volitional preactional stage are motivated to change, but they do not act because they might lack the right skills to translate their intention into action. Planning is a key strategy at this point. It serves as an operative mediator between intentions and behavior.
Principle 4: Two kinds of mental simulation. Planning can be divided into action planning and coping planning. Action planning pertains to the when, where, and how of intended action. Coping planning includes the anticipation of barriers and the design of alternative actions that help to attain one’s goal in spite of impediments.
Principle 5: Phase-specific self-efficacy. Perceived self-efficacy is required throughout the entire process. However, the nature of self-efficacy differs from phase to phase. This is because there are different challenges as people progress from one phase to the next one. Goal setting, planning, initiative, action, and maintenance all pose challenges that are not of the same nature. Therefore, we distinguish between preactional self-efficacy, coping self-efficacy, and recovery self-efficacy. Sometimes the terms task self-efficacy instead of preaction self-efficacy, and maintenance self efficacy instead of coping and recovery self efficacy are preferred.
Assessment of Constructs
Risk Perception. Risk perception can be measured by items such as “How high do you rate the likelihood that you will ever get one of the following diseases: (a) cardiovascular disease (e.g., heart attack, stroke), (b) diseases of the musculoskeletal system (e.g., osteoarthritis, herniated vertebral disk)?” Any other health risk can be added, if relevant to the research context.
Outcome Expectancies. Positive outcome expectancies (pros) and negative outcome expectancies (cons) can be assessed, for example, with the stem “If I engage in physical activity at least three times per week for 20 minutes . . .” followed by pros such as “then I feel better afterwards,” or “then I meet friendly people,” and followed by cons such as “then every time would cost me a lot of money,” or “then I would be financially depleted.”
Self-efficacy. Perceived motivational and volitional self-efficacy can be composed of items such as the following. Motivational self-efficacy (task self-efficacy) refers to the goal-setting phase and can be measured with the stem “I am certain . . .” followed by items like “that I can be physically active on a regular basis, even if I have to mobilize myself,” or “that I can be physically active on a regular basis, even if it is difficult.” Volitional self efficacy refers to the goal-pursuit phase. It can be subdivided into coping self-efficacy and recovery self-efficacy. Coping self-efficacy has been measured with the stem “I am capable of strenuous physical exercise on a regular basis . . .” followed by barriers like “even if it takes some time until it becomes routine,” or “even if I need several attempts until I will be successful.” Items on recovery self-efficacy can be worded “I am confident that I can resume a physically active lifestyle, even if I have relapsed several times,” “I am confident that I am able to resume my regular exercises after failures to pull myself together,” or “I am confident that I can resume my physical activity, even when feeling weak after an illness.”
Intention. Intention to perform a behavior is assessed in correspondence to the behavior itself: for example, “I intend to perform the following activities at least 3 days per week for 20 minutes: strenuous (heart beats rapidly, sweating) physical activities,” “moderate (not exhausting, light perspiration) physical activities,” and “mild (minimal effort, no perspiration) physical activity.” Answers can range, for example, from not at all true (1) to absolutely true (6). Alternatively, intention can be assessed in terms of frequency and duration of more specific behaviors: (a) physiotherapeutic exercises (e.g., back training), (b) fitness activities (e.g., using an exercise bike), (c) resistance training (training muscle strength, e.g., on machines), and (d) physical activity while commuting (e.g., going by bicycle or walking for longer distances).
Planning. Action Planning can be assessed with items addressing the when, where, and how of the activity: for example, “I have already planned . . .” (1) “which physical activity I will perform (e.g., walking),” (2) “where I will be physically active (e.g., in the park),” (3) “on which days of the week I will be physically active,” and (4) “for how long I will be physically active.” Coping planning, on the other hand, can be measured with the item stem “I have made a detailed plan regarding . . .” and the items (1) “what to do if something interferes with my plans,” (2) “how to cope with possible setbacks,” (3) “what to do in difficult situations in order to act according to my intentions,” (4) “which good opportunities for action to take,” and (5) “when I have to pay extra attention to prevent lapses.” Another option is to ask participants to actually generate their plans, which, however, confounds measurement and treatment.
Action Control. While planning is a prospective strategy, that is, behavioral plans are made before the situation is encountered, action control is a concurrent self-regulatory strategy, where the ongoing behavior is continuously evaluated with regard to a behavioral standard. Action control can be assessed with a six-item scale comprising three facets of the action control process: selfmonitoring (“I consistently monitored myself whether I exercised frequently enough,” or “I consistently monitored myself when, where, and how long I exercise”), awareness of standards (“I have always been aware of my prescribed training program,” or “I often had my exercise intention on my mind”), and self-regulatory effort (“I really tried hard to exercise regularly,” or “I took care to practice as much as I intended to”).
Staging. When using the continuum model for the prediction of behavior, these variables are being specified as predictors and mediators in a path model (see Figure 1). When employing the stage variant to conduct an intervention study, an assessment of stages is necessary. Stage theories employ algorithms for the staging procedure which can be regarded as a fast and frugal tree with satisfactory validity. For a three-stage procedure, one needs two steps. First, behavior is assessed on the basis of a context-specific dichotomous criterion (yes = already active, no = not yet sufficiently active). Those who meet the preselected criterion are defined as actors. Those who don’t are subject to the second step by asking them whether they intend to become active or not. If they do intend, they are defined as intenders; if they don’t, they are nonintenders (or preintenders). Such straightforward diagnostic procedures may be too simple to account for response bias and temporal fluctuation. However, when subdividing large samples to assign stage-matched treatments, such a pragmatic procedure results in more homogeneous subgroups that allow for more effective interventions.
Conclusion
In sum, the HAPA has two layers: a continuum layer and a phase (or stage) layer. Depending on the research question, one might choose one or the other. HAPA is designed as a sequence of two continuous self-regulatory processes, a goalsetting phase (motivation) and a goal-pursuit phase (volition). The second phase is subdivided into a preaction phase and an action phase. One can superimpose these three phases on the continuum model as a second layer and regard phase as a moderator.
This two-layer architecture allows switching between the continuum model and the stage model, depending on the given research question. The stage layer is useful for designing stage-matched interventions. For preintenders, one needs risk and resource communication, for example by addressing the pros and cons of a critical behavior. For intenders, planning treatments are helpful to support those who lack the necessary skills to translate their intentions into behavior. And for actors, one needs to stabilize their newly adopted health behaviors by relapse prevention strategies.
The HAPA allows both the researcher and the practitioner to make a number of choices. Although it was initially inspired by distinguishing between a motivational and a volitional stage, and later expanded to the distinction between preintenders, intenders, and actors, one need not necessarily group individuals according to such stages. If the purpose is to predict behavior change, one would specify a mediator model that includes postintentional constructs (such as planning and volitional self-efficacy) as proximal predictors of performance.
For stage-tailored interventions, however, usually three stage groups would be established. This does not exclude the possibility of generating more than three stages. For example, for some research questions, one might subdivide the preintenders into precontemplators and contemplators, according to the TTM. Or one might opt for a distinction between preintenders, who are (a) unaware of an issue, (b) aware but unengaged, or (c) still deciding. Thus, HAPA is not a puristic stage model, but a principle-based framework that allows for a variety of approaches. Evidence from intervention studies shows good results, in particular for patients with various chronic illnesses and disabilities. Planning interventions and action control programs proved especially successful.
References:
- Fleig, L., Lippke, S., Pomp, S., & Schwarzer, R. (2011). Exercise maintenance after rehabilitation: How experience can make a difference. Psychology of Sport and Exercise, 12, 293–299. doi: 10.1016/j.psychsport .2011.01.003
- Gellert, P., Ziegelmann, J. P., & Schwarzer, R. (2012). Affective and health-related outcome expectancies for physical activity in older adults. Psychology & Health, 27, 816–828. doi: 10.1080/08870446.2011.607236
- Heckhausen, H., & Gollwitzer, P. M. (1987). Thought contents and cognitive functioning in motivational versus volitional states of mind. Motivation and Emotion, 11, 101–120.
- Lippke, S., Ziegelmann, J. P., Schwarzer, R., & Velicer, W. F. (2009). Validity of stage assessment in the adoption and maintenance of physical activity and fruit and vegetable consumption. Health Psychology, 28, 183–193. doi: 10.1037/a0012983
- Luszczynska, A., Schwarzer, R., Lippke, S., & Mazurkiewicz, M. (2011). Self-efficacy as a moderator of the planning-behaviour relationship in interventions designed to promote physical activity. Psychology & Health, 26, 151–166. doi: 10.1080/08870446.2011.531571
- Parschau, L., Richert, J., Koring, M., Ernsting, A., Lippke, S., & Schwarzer, R. (2012). Changes in socialcognitive variables are associated with stage transitions in physical activity. Health Education Research, 27, 129–140. doi: 10.1093/her/cyr085
- Prochaska, J. O., & DiClemente, C. C. (1983). Stages and processes of self-change of smoking: Toward an integrative model of change. Journal of Consulting and Clinical Psychology, 51, 390–395.
- Scholz, U., Nagy, G., Schüz, B., & Ziegelmann, J. P. (2008). The role of motivational and volitional factors for self-regulated running training: Associations on the betweenand within-person level. British Journal of Social Psychology, 47, 421–439.
- Schwarzer, R. (1992). Self-efficacy in the adoption and maintenance of health behaviors: Theoretical approaches and a new model. In R. Schwarzer (Ed.), Self-efficacy: Thought control of action (pp. 217–243). Washington, DC: Hemisphere.
- Schwarzer, R. (2008). Modeling health behavior change: How to predict and modify the adoption and maintenance of health behaviors. Applied Psychology, 57, 1–29.
- Sniehotta, F. F., Schwarzer, R., Scholz, U., & Schüz, B. (2005). Action planning and coping planning for longterm lifestyle change: Theory and assessment. European Journal of Social Psychology, 35, 565–576.
- Wiedemann, A. U., Lippke, S., Reuter, T., Ziegelmann, J. P., & Schüz, B. (2011). The more the better? The number of plans predicts health behaviour. Applied Psychology: Health & Well-Being, 3, 87–106. doi: 1111/j.1758-0854.2010.01042.x
See also: