Tremendous advances in medical technologies and the emergence of neonatology as a medical specialty have led to the increase in the number of surviving high-risk infants. The developmental status of these children is of great concern to a wide range of professionals. Special educators, school psychologists, developmental psychologists, early childhood educators, and speech and language pathologists are now dealing with a new category of special children. Although the physician is primarily concerned with mortality and morbidity factors, other professionals are interested in developmental performance, family concerns, speech and language development, and later school achievement.
Definitions, Factors, And Incidence
The term high risk encompasses a class of infants who have been exposed to any one of a number of medical factors that may contribute to later developmental delay. These are infants who have been subjected to a potent array of potentially debilitating conditions. Children are identified as being at high risk for developmental difficulties if they experience problems before, during, or after birth that are known to be associated with later difficulties in development. Reviews of the high-risk population can be confusing because of the multiple and overlapping factors that place an infant at risk.
Clarification of Terminology: Birth Weight and Gestational Age
Gestational age and birth weight are most often mentioned in high-risk issues and are defined using World Health Organization criteria. These are barometers for developmental risk and provide an objective means of establishing risk status. A full-term infant is one born between 37 and 41 weeks of gestational age, and infants who are born before 37 weeks of gestational age are defined as premature. Premature infants usually weigh less than 2,500 g (5 lb, 8 oz) and constitute 12% of all births in the United States. Infant mortality rises from five times normal at 37 weeks of gestational age to 45 times normal at 32 weeks of gestational age. Most of the problems associated with prematurity occur in infants with birth weights of 1,500 g (3 lb, 5 oz) or less, usually in those born at less than 32 weeks of gestational age. Incidence rates for neurological and developmental delay for this group range from 18 to 80%, depending on the assessments used.
Birth weights of less than 2,500 g are labeled low birth weight, and very low birth weight is designated for infant weights less than 1,500 g. Together, birth weight and gestational age provide a more accurate means of determining an infant’s risk status. Infants born before term are usually also low in birth weight. It is important to distinguish between those infants whose birth weight is close to what would be expected, given their early delivery date, and those whose weight is lower than would be expected. In addition to classifications of appropriate for gestational age (AGA) and low birth weight (LBW and VLBW), another classification of small for gestational age (SGA) combines the two terminologies. Full-term infants may also be SGA, and therefore at risk for postnatal difficulties. Risks are greater for SGA babies than for babies born early but appropriate in size. Generally, the risk for infant mortality increases as birth weight and gestational age decrease.
Extreme prematurity and very low birth-weight are known to be associated with developmental problems. Developmental problems may be temporary delays or impairments associated with illness or environmental conditions, or they may be indications of long-term developmental conditions. Researchers have noted that roughly 15% to 40% (depending on how the group is selected and what kind of problems are considered) of extremely premature infants have significant, long-term medical or developmental problems.
In summary, a high-risk infant is an infant who, because of low birth weight, prematurity, serious medical complications, or adverse environmental conditions, has a greater than average chance of displaying developmental delay or later cognitive or motor deficits or a combination of these in the neonatal or postnatal period. The definition of the risk is necessarily broad because there is increasing evidence that the quality of familial, medical, therapeutic, and educational care that is provided to the child immediately following birth has great influence on the quality of that child’s life.
Incidence of High-Risk Infants
Before the advent of the neonatal intensive care unit (NICU), the risk for neonatal death was 30 times greater for low-birth-weight infants. The NICU has greatly modified the concept of risk because many more infants now survive because of the environment it provides immediately following birth. This is reflective in the changes from neonatal mortality statistics (death within the first month of life) in the 1960s (21 deaths per 1,000 births); the 1970s (15 deaths per 1,000 births); the 1980s (18 deaths per 1,000 births); and the 1990s (5 deaths per 1,000 births). The creation of the NICU has reduced the neonatal mortality rate but at the same time increased the number of surviving infants who are at risk for developmental delays. Saving very small and very sick infants results in a greater incidence of handicapping conditions. Estimates of incidence of high-risk infants range from 5% to 15% of all newborns, depending on the classification criteria. The inclusion of congenital anomalies in the description helps to differentiate between earlier and later babies, with the incidence of anomalies at 2.3% for babies born at 40 or 41 weeks and 30% for babies born before 28 weeks of gestation.
Infants at risk for delay also tend to come from nonwhite families, and this is related to socioeconomic status. For example, in the new millennium, black infant neonatal mortality rates (13%) continue to be almost twice the rate of white infants (8%). These statistics reflect the lack of prenatal care available to low-income families in the United States as well as the risk factors related to mother’s age and behavior during pregnancy; these will be discussed later in this entry.
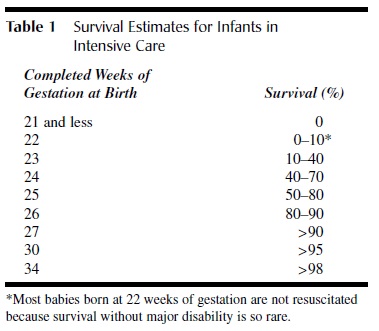 Table 1 Survival Estimates for Infants in Intensive Care
Table 1 Survival Estimates for Infants in Intensive Care
Survival
Many factors increase an individual baby’s chances of survival. The most important of these are the baby’s gestational age and weight; the absence of breathing problems; the absence of congenital abnormalities; and the absence of other severe diseases, especially infection. In the smallest infants, gestational age is usually most important because it determines whether the infant’s organs, particularly the lungs, have developed enough to allow the baby to live within the limits of current technology.
General estimates of survival for live-born infants who receive neonatal intensive care in the United States in the new millennium are noted in Table 1.
Assessment
Immediate Neonatal Assessments
There are special exams conducted in the NICU that examine a high-risk infant’s behavior to get a picture of how he or she acts and reacts to stimuli and the surroundings. What is learned from the exam can be used to make the baby’s world fit his or her own special needs. The exams assess if and how quickly the baby becomes awake and alert; how the baby soothes himself or herself when upset and how easy it is for an adult to soothe the baby; the baby’s movement patterns; and how much handling the baby can tolerate without becoming upset.
The Apgar scoring system measures a newborn infant’s physical responsivity, development, and overall state of health shortly after birth. The exam measures heart rate, breathing, muscle tone, reflex response, and color, which reflect the newborn’s adaptation to life outside the womb. Because of their early birth, highrisk premature babies are more likely to have lower Apgar scores. Depending on the maturity of the infant’s lungs, the newborn may have trouble breathing. Breathing and heart rate can be assessed using a cardiorespiratory monitor. Incubators are also used to warm premature babies who have less body fat.
The Brazelton Neonatal Behavioral Assessment Scale (NBAS) is an interactive assessment of the newborn’s behavioral repertoire and neurological responses during the neonatal period. Assessments of physiological, motor, state, interactive and attentional, and self-regulation functions are made, and observations of the infant’s communicative signals are included.
Routine developmental screenings during the first 2 years are then plotted from the infant’s estimated due date rather than the infant’s birth date. The Denver Prescreening Developmental Questionnaire, the Denver Developmental Screening Test, and the Gesell Screening Inventory are all examples of standardized developmental tests. These forms of screening do not replace neurologic examinations. Because of this, standardized examinations, such as the Neonatal Neurodevelopmental Examination, have been developed and are used primarily by developmental pediatricians and pediatric neurologists. The Neonatal Neurodevelopmental Examination assesses postural reflexes and muscle tone, cranial nerve and motor function, sensory responses, and behavior.
Long-Term Assessments
For long-term developmental assessments beyond infancy, it becomes difficult to make a list of definitive developmental milestones that must be met by a certain date. The range of how children do things and when they accomplish developmental tasks becomes broader, largely owing to the increasing influence of culture and experience. The results from testing infants and young children do not reveal how they may do at school age or later in life. There are a number of reasons it is difficult to predict later levels of functioning from testing done with infants and young children, including the fact that the most critical skills tested in older children and adults do not yet exist in infancy.
Another reason why infant tests cannot predict future success involves the importance of later events in determining a child’s progress. For example, a young child may have a sensory impairment or motor problem that would profoundly affect performance and limit access to what he or she knows. Later correction or adaptation for the impairment (e.g., glasses, hearing aids, braces) may provide a dramatic difference in the course of the child’s progress.
Finally, developmental problems tend to emerge slowly over time as higher levels of brain functioning are called into use. Injury to areas of the brain important for later functioning may not be apparent in an infant or very young child. It is important to look at high-risk children frequently over time to identify delays in their development compared with age mates. Identifying delays early allows for investigation into causes and referral to therapies that may be able to improve or stabilize skills. It is also helpful to compare a child’s current performance to his or her previous pattern of development to document the rate of change and recovery being made.
In general terms, developmental evaluations assess how well a child is developing for his or her age. A child’s test scores are compared with the average scores for children of the same age. The areas tested include language skills, attention, social behavior, thinking and problem solving, and fine and gross motor skills. These evaluations should also take into consideration the quality of the child’s performance, including completion, approach, ease, frustration, and general response, which can help in understanding how the child may be helped most successfully.
Physical Components Of High Risk
The initial physical elements of high-risk status are often discussed as risk factors. Risk factors are defined as characteristics of the infant, the caregiver, or the life situation that have the potential for harming development. When risk factors are in operation, the result may be poor socialization, later problems with mental health, and poor school performance. Risk factors usually occur in multiples, making it difficult to discover the nature of their effect on the infant’s development. Certain risk factors tend to be accompanied by specific other factors, which is termed comorbidity. For example, a baby with fetal alcohol syndrome is often being cared for by a mother who continues to abuse alcohol, and the mother’s negligence and abusiveness are comorbid with the infant’s physical condition. Not all the risk factors for an individual are necessarily present at birth or even at age 2. Although early risk factors can be powerful, later events can play a real part in determining how well a child or adult functions.
Birth Risk Factors
Although many factors may place an infant at risk for developmental disabilities, those related to the birth process are most closely associated with later difficulties. Infants born too soon or too small are at risk for a number of problems. First, they may have difficulty adapting to the postnatal environment owing to their less mature body organs, especially their lungs. Second, they may have restricted growth potential. Third, they may exhibit certain biochemical or physiological disturbances that place them at risk for brain damage. Finally, they may be born into an environment in which certain socioeconomic factors combine with the physical factors of prematurity to double their chances of risk.
Maternal Factors
Maternal histories that include premature births, repeated miscarriage, cervical incompetence, still birth, uterine and placental abnormalities, intrauterine growth retardation, blood group problems, unexplained fetal or neonatal death, and genetic disease or chromosomal disorders may lead to higher risk potentials. Substance abuse (including smoking and alcohol use) and malnutrition are other factors that have been well linked to poor birth outcomes. Medical conditions can also contribute to early labor, including premature rupture of the membranes, which can place mother and baby at increased risk of infection; prolonged labor; uncontrolled delivery; or an abnormal presentation.
Immediate Post-birth Physical Concerns
High-risk preterm infants can experience a higher rate of respiratory, neurological, and gastrointestinal problems that affect general developmental problems. A number of physical functions affect each other, and when one goes wrong, other linked physical problems may follow. Immediate post-birth concerns include the monitoring of immature lungs that are likely to suffer from respiratory distress syndrome and periods of apnea. Respiratory distress syndrome arises when the infant’s lungs are too immature to successfully guide the exchange of oxygen and carbon dioxide. Unfortunately, mechanical ventilation, which essentially blows air under pressure into the lungs, can, in turn, cause irritation and long-term lung damage.
Poor fetal circulation may occur, bringing on hypoxia. At times of hypoxia, the infants’ body directs blood to the brain and away from the lower part of the body. As a result, the poor supply of blood to the intestines may lead to necrotizing enterocolitis (gangrene of the intestines), which must be treated surgically. Brain damage as a result of brain bleeds can be related to the difficulties in breathing and in blood circulation. Finally, premature high-risk newborns are also likely to have dangerously high bilirubin, which can be treated with medication and with phototherapy using ultraviolet light.
In summary, high-risk infants may spend many weeks in the NICU, where they are necessarily subjected to many invasive procedures; they must often be fed by tube through the nose or mouth, have their breathing artificially assisted, and receive medications or fluids intravenously. Technology has become so advanced that most infants could be kept alive indefinitely with assistance in breathing, artificial feeding, and even kidney dialysis. This calls into consideration difficult questions of whether life alone is the highest priority, or whether quality of life is a greater concern.
In addition to these aspects, there may be complications that some prematurely born children experience in the NICU. Continued short and long-term health problems for premature infants can include feeding and growth problems because of an immature digestive system, anemia, infections, and general failure to thrive.
For any infant, it is impossible to predict the likelihood of a significant handicap (moderate or severe mental retardation, inability to walk without assistance, blindness or deafness). However, some factors increase the risk for these handicaps: extreme prematurity, identifiable brain abnormalities, and lengthy periods of illness. It is necessary to understand the limitations of trying to use information available during infancy and early childhood to predict later development. Some aspects of development are affected by experience; other aspects of development will unfold at the rate they would have if the child had been born at term.
Continued Childhood Disabilities
Children who are born prematurely have an increased risk for early brain injury that is often associated with developmental difficulties. Motor symptoms are usually the earliest manifestation of early neurological injury. These symptoms may resolve as the child recovers, or they may eventually be diagnosed as cerebral palsy. Although early identification is necessary for early intervention, it can be very difficult to establish clear diagnoses of neurodevelopmental problems in developing infants.
During childhood, health difficulties can continue in the form of frequent illnesses. Minor disabilities during school age may result, which include short attention span; specific learning problems in school, such as difficulty with math or reading; language delays; low intelligence test scores; deficits in motor coordination and school learning; and poor emotional adjustment. Generally, children with these relatively minor disabilities lead normal lives.
Social Components: Family Issues
During this stressful time of infant diagnosis, parents may unknowingly worsen the situation. Separate from the physical elements are the social elements of high risk. From the very beginning, there are many reasons to be concerned about the high-risk infant’s early social environment. In most physical high-risk situations, parents are unable to be with their babies in the same way, particularly if life-supporting technology is involved. Hospital isolettes provide the baby support, but the necessary physical separation can interfere with parent-infant bonding. Hospital procedures can delay opportunities to hold and interact with the baby in semiprivate settings.
Parents may have their own personal concerns around past experiences that can affect bonding with the high-risk baby. Even the baby’s characteristics can affect bonding, such as the baby’s health, physical defects, alertness, and responsiveness. Each of these has potential to interfere with eye contact or with facial expression, which are key to developing a bond between infant and parent.
Concerns about parental competence certainly overwhelm parents. These areas include providing physical care, physical protection, and psychological support; controlling, motivating, and regulating children’s behavior; and teaching and providing knowledge and skills in a loving environment. These, in addition to the stress of having a high-risk infant, along with financial concerns, can add to these overwhelming feelings.
Psychosocial Concerns for Families
In addition to bonding and social stressors, there may be psychosocial issues on the part of family members that can affect the high-risk infant. First, high-risk pregnancies and low birth weight are most common among low-income women, especially women of color. These mothers are more likely to be undernourished and live in conditions that expose them to harmful environmental influences such as pollution, unsafe housing, and chemical exposures. Further, they may have less access and experience more barriers that keep them from receiving the prenatal care necessary to protect them and their babies. Maternal psychological status during pregnancy can also be a risk concern, which may include unwanted pregnancy, lack of support, and psychiatric disorders. These psychological issues may manifest themselves in drug or alcohol use, mental illness, or depression. Other psychosocial concerns, including parental issues about attachment and loss, adolescent-aged parents, and extreme situations involving violence, can affect the social environment of an infant, whether high risk or not.
Second, a difficult infant may be so frustrating to the caregivers that they spend less time interacting with him or her. The infant’s poor social competence may also put him or her at risk, particularly if the infant is incapable of expressing needs to adults. Risks are greater when the infant shows low readability, low predictability, and low responsiveness to adults.
Finally, experiences that occur by chance may also affect the family or infant alone. Sudden and too-frequent changes from familiar to unfamiliar situations can be stressful for the infant. Other extreme experiences, such as the death of a parent or separation after attachment has taken place, can negatively affect the infant. Risk is more evident when the separation is abrupt and prolonged, and can be seen in the infant in the forms of protest, despair, and then detachment.
Psychosocial Coping With Stress
Caring for a premature infant can be a great challenge, which can naturally bring on anxiety about the baby’s health and feelings of anger, guilt, or depression. Postpartum depression and physical recovery from birth, in addition to caregiving stresses, can lead to overwhelming fatigue. Some suggestions for parents may help during this difficult time:
- Learn everything you can about your baby’s condition. In addition to talking to your doctor and your baby’s caregivers, read books on premature birth and look for information on the Internet.
- Take care of yourself, providing yourself with rest and good nutrition to feel stronger and better able to care for your baby.
- Seek good listeners for support, including partners, friends, family members, or premature baby support groups.
- Accept help from friends and family to help save your energy for your baby.
- Keep a journal. Record the details of your baby’s progress as well as your own thoughts and feelings. Include pictures of your baby, so that you can see how much he or she is changing.
Strategies To Decrease Risk: Interventions
Most high-risk premature infants eventually develop beyond any negative consequences associated with prematurity. Close attention to developmental needs can help lessen any long-term impact of the temporary developmental problems many premature infants experience. For children who develop long-term conditions as a result of early medical complications, immediate interventions can reduce the eventual level of disability.
Perinatal Services
Perinatal services must be provided as quickly as possible to minimize disability by identifying possible conditions requiring further evaluations, diagnosis, and treatment. Early intervention programs often take place in the neonatal nursery, at home, and at special centers. In addition to early screening assessments (reviewed earlier), special attention may be given to the handling of the newborn. A form of holding encouraged in many NICUs is known as kangaroo care, the skin-to-skin contact between infant and caregiver. This form of holding was adopted from countries where isolettes to keep preterm infants warm are scarce. Studies show that the mother’s body temperature adjusts to keep the baby’s temperature at the right level. The baby’s breathing also becomes more even, and heart rate and blood oxygen levels stay steady. Also, giving the stable infant gentle massage for short periods daily has been shown to help babies gain weight faster.
Perinatal services also may provide parents training in infant caregiving skills: when effective stimulation helps preterm babies develop, parents are likely to feel encouraged and interact with the baby more effectively. For example, home visit programs include multiple visits, during which physical exams and developmental screenings are administered by nurses. Evaluations of homes for infant safety, providing health and parent education, and reinforcing hospital discharge treatment instructions are also part of these programs. Nurses also provide referrals to other public health and community social services that can assist the family. At each visit, the infant’s physical, developmental, psychosocial, cognitive, and emotional growth is assessed so that any need for further services can be identified quickly. Studies have found that those receiving home visits had fewer life-threatening illnesses, fewer hospital admissions, fewer intensive care admissions, and fewer days in the intensive care unit than those not receiving the program.
Developmental Care for the Newborn
Another widely used strategy for working with high-risk newborns is developmental care. Developmental care is designed to prevent the brain from being injured by intense or painful stimulation, and to provide the kinds of everyday experiences that will help the baby to develop normally. A major goal of developmental care is to protect the high-risk infant’s brain and central nervous system, which control the five areas of development (physiological, motor, sleep/wakefulness, attention, and self-regulation) that are the base for the baby’s motor, mental, and social development.
Studies of developmental care have shown that by making the NICU world more “baby friendly,” some of these problems can be prevented. The physical environment can be changed to reduce the amount of sound and light, provide some support for the baby’s position because he or she cannot get into a comfortable position alone, make treatments less stressful and frequent, and provide gentle handling by pacing the care according to how the baby reacts.
Through the developmental care approach, parents are taught to become attentive to the many ways an infant interacts with those around him or her: by looking, listening, and touching and feeling. When the baby attends, he or she focuses on and follows things and makes eye contact. This approach can easily be incorporated into discharge planning from the NICU. Important aspects include the parents’ involvement in their infant’s care, plans for special needs such as oxygen and apnea monitoring, and teaching the parents special skills such as cardiopulmonary resuscitation.
With the realization that the parents are undergoing transitional stress that may interfere with their ability to learn, parental education is often reinforced after the infant’s discharge. This educational programming includes developing parenting skills, helping parents build close affectionate ties to their infants so that they will be attuned to their babies’ special needs, and encouraging the family to work together, particularly during crises and decision making.
Continued Care for Toddlers
As the high-risk infants develop into toddlers, specific skill areas such as vision, speech, and hearing will continue to be examined as well as overall developmental performance. During this developmental period, preschoolers develop, modify, and master skills in the areas of motor performance, cognitive development, social awareness, and language functioning. Toddler intervention programs have the following general characteristics: (1) orientation to prevention of developmental delay; (2) orientation to changes in the infant’s behavior, development, or relations with caregivers; and (3) focus on change within the family system to foster positive changes in the child.
Prenatal Prevention
Perhaps the best treatment for preterm and low birth-weight infants is before the actual birth. Prevention in the form of focused self-care, regularly scheduled prenatal care visits, proper nutrition, avoiding any exposure to tobacco smoke, avoiding alcohol and illegal substances, and control of chronic medical problems are all ways that women can help maintain a healthy pregnancy to the full term.
In summary, high-risk infants face many developmental challenges that are caused by multiple factors. Given the high numbers of high-risk infants in the United States, many public health strategies have focused on prevention and early intervention with hopes of encouraging and funding multidisciplinary approaches to risk reduction during pregnancy and education of the general population about modifiable risk factors for and consequences of low birth weight.
References:
- Center for the Future of Children. (1995). The future of children: Low birth weight (Vol. 5, pp. 176 –196). Princeton, NJ: Brookings
- March of Dimes, http://www.modimes.org
- Parents of Premature Babies, , http://www.Preemie-L.org
- Rossetti, L. (1989). High-risk infants: Identification, assessment and intervention. Boston: College Hill
- Widerstrom, H., Mowder, B. A., & Sandall, S. R. (1991).At-risk and handicapped newborns and infants. Development, assessment and intervention. Englewood Cliffs, NJ: Prentice Hall.